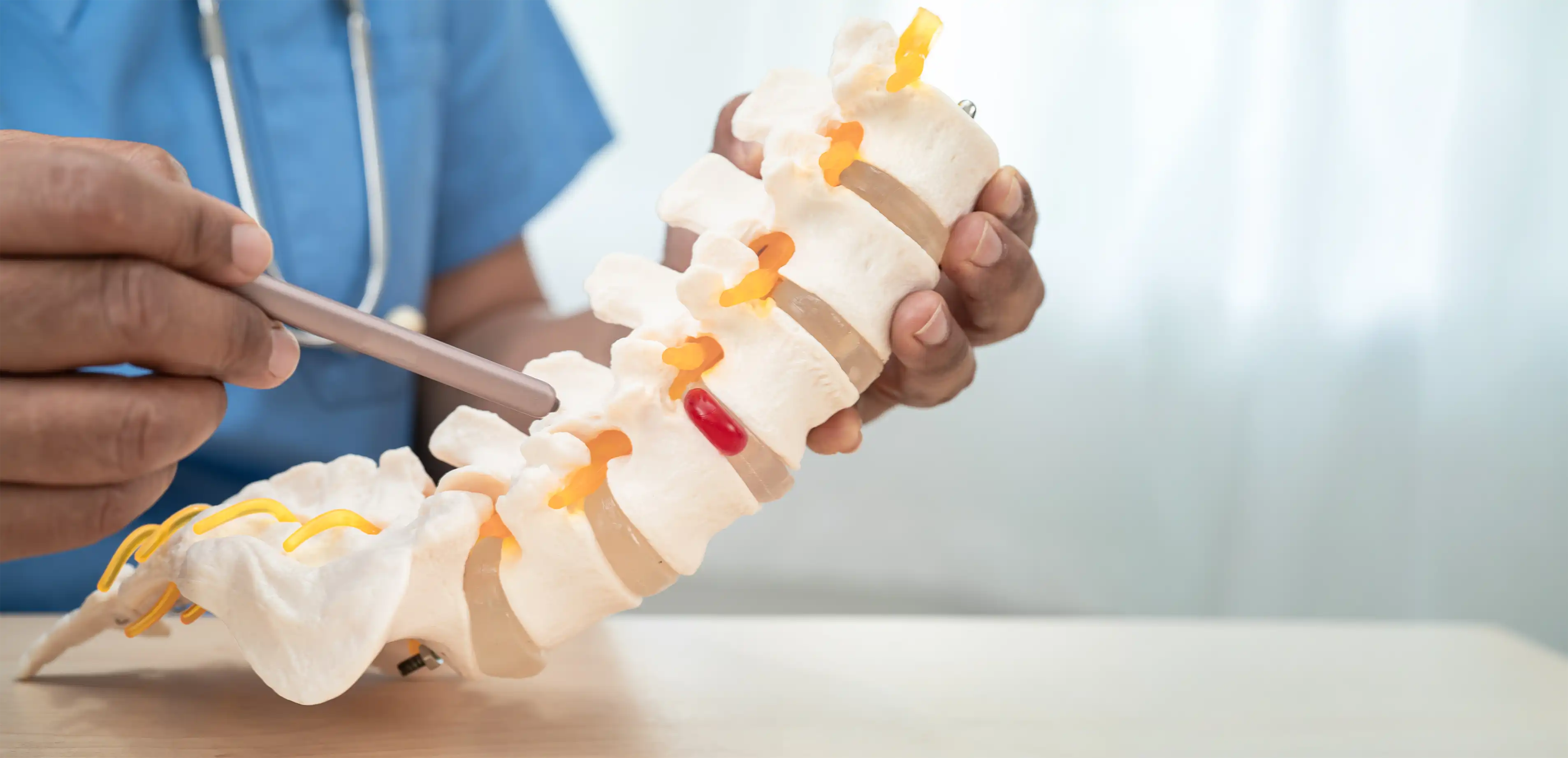
A disc prolapse, also known as a herniated disc or slipped disc, occurs when the soft, gel-like center of an intervertebral disc pushes through a tear in its outer fibrous layer. This condition can place pressure on nearby nerves, leading to pain, neurological symptoms, and reduced mobility.
Disc prolapse can occur in different regions of the spine, most commonly in the lumbar spine (lower back) or the cervical spine (neck).
At Fakeeh University Hospital Dubai, our spine specialists provide comprehensive evaluation and personalized treatment for patients with disc prolapse. Using advanced diagnostic imaging and minimally invasive surgical techniques when necessary, we focus on relieving nerve compression, restoring spinal function, and helping patients return to their daily activities.
Early diagnosis and appropriate treatment are essential to prevent persistent nerve irritation and long-term complications.
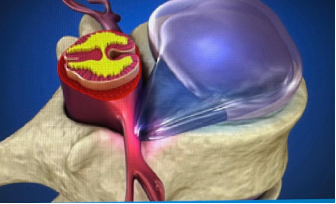
The spine is composed of vertebrae separated by intervertebral discs, which act as shock absorbers and allow flexibility of the spine.
Each disc contains:
A disc prolapse occurs when the inner material pushes through a tear in the outer layer. If the protruding disc material compresses nearby nerves or the spinal cord, it can cause pain and neurological symptoms.
Disc prolapse most frequently occurs in:
Symptoms depend on the location and severity of the disc herniation.
Common symptoms include:
Lumbar disc prolapse commonly causes sciatica, where pain travels down the leg.
Cervical disc prolapse may cause arm pain, weakness, or sensory changes.
Disc prolapse usually develops due to a combination of age-related degeneration and mechanical stress on the spine.
With aging, spinal discs gradually lose hydration and elasticity. This natural wear and tear makes the disc more vulnerable to tears and herniation.
Activities involving repetitive bending, lifting, or twisting place increased stress on spinal discs.
Occupations that require heavy lifting or prolonged physical strain may increase the risk.
Sudden trauma, such as falls, accidents, or sports injuries, can cause an acute disc rupture.
Long periods of sitting, especially with poor posture, can place excessive pressure on spinal discs and contribute to degeneration over time.
Several factors increase the likelihood of developing a disc prolapse:
Maintaining a healthy lifestyle and proper spinal mechanics can reduce the risk.
At Fakeeh University Hospital Dubai, diagnosis begins with a comprehensive evaluation.
During the consultation, the physician evaluates symptoms, neurological function, reflexes, muscle strength, and spinal mobility.
Specific tests may help determine whether nerve roots are being compressed.
Imaging tests are often used to confirm the diagnosis and determine the exact location of the disc herniation.
These may include:
Accurate diagnosis allows targeted and effective treatment.
Treatment depends on symptom severity, neurological findings, and the patient's overall condition.
Most patients improve with conservative treatment.
Targeted physiotherapy helps strengthen spinal muscles, improve flexibility, and reduce pressure on affected nerves.
Pain-relieving and anti-inflammatory medications may help reduce inflammation and nerve irritation.
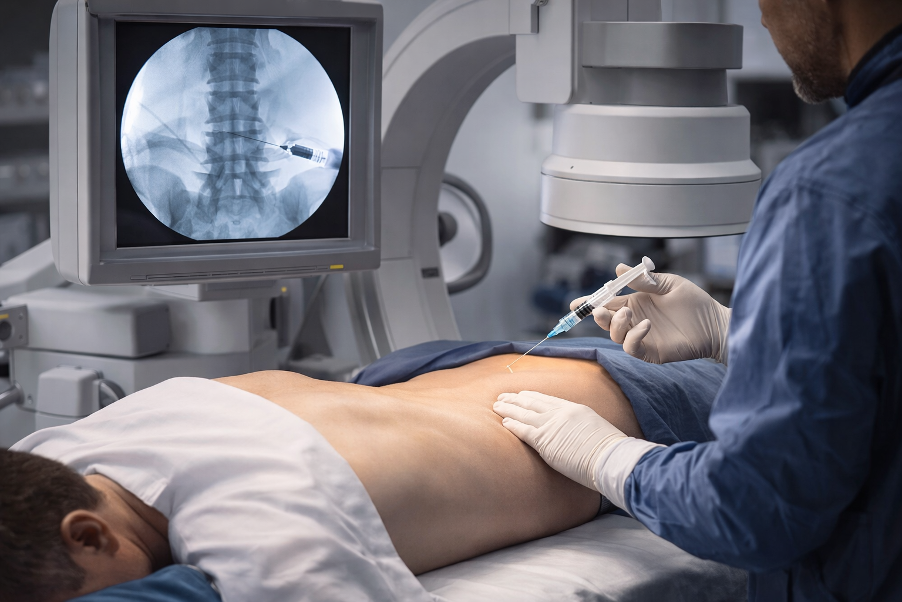
Image-guided spinal injections may be used to reduce inflammation around irritated nerve roots and provide pain relief.
Surgery may be recommended if:
When surgery is necessary, we use advanced minimally invasive techniques, including:
• Microscopic discectomy
• Endoscopic spine surgery
These procedures allow precise removal of the herniated disc material while minimizing tissue disruption, leading to faster recovery and earlier patient discharge.
The surgical technique is carefully selected based on the specific findings of each case.
.jpg)

With appropriate treatment, most patients recover well from disc prolapse and can return to normal activities.
Early diagnosis and targeted therapy are important to prevent chronic nerve irritation and long-term complications.
Immediate medical evaluation is necessary if symptoms include:
These may indicate serious neurological compression and require urgent treatment.
If you are experiencing persistent neck pain, back pain, or radiating arm or leg symptoms, early evaluation can help identify the underlying cause and guide effective treatment.
Book your appointment at Fakeeh University Hospital Dubai to receive expert diagnosis and personalized spine care.

Spinal disc prolapse — also commonly known as a slipped disc, herniated disc, or ruptured disc — occurs when the soft, gel-like inner core of an intervertebral disc (the nucleus pulposus) pushes through a tear or weakness in the tough outer layer (the annulus fibrosus). This displaced disc material can press against nearby spinal nerves or the spinal cord itself, causing pain, numbness, or weakness.
Common causes of disc prolapse include:
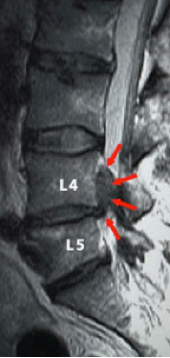
Disc prolapse most commonly affects the lumbar spine (lower back) — particularly at the L4–L5 and L5–S1 levels — but can also occur in the cervical spine (neck).

Symptoms of disc prolapse vary depending on the location and severity of the prolapse, and which nerves are affected. Common symptoms include:
Lower back disc prolapse (lumbar):
Neck disc prolapse (cervical):
Important: If you experience sudden loss of bladder or bowel control, severe progressive weakness in both legs, or numbness in the inner thighs and groin — seek emergency medical care immediately. These are signs of cauda equina syndrome, which requires urgent surgical intervention.

This is one of the most common questions patients ask — and the answer is important to understand.
Standard X-ray alone cannot directly show a disc prolapse. Here is why:
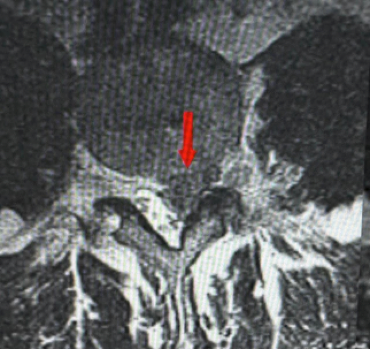
The gold standard imaging for disc prolapse is MRI:
CT scan may be used when MRI is not available or contraindicated, and CT myelography can be used in complex cases.
At Fakeeh University Hospital Dubai, our radiology team provides advanced MRI and CT imaging with specialist reporting for accurate disc prolapse diagnosis.

Treatment of disc prolapse depends on the severity of symptoms, the degree of nerve compression, and how long symptoms have been present. Most cases improve with conservative management — surgery is reserved for specific indications.
Conservative (Non-Surgical) Treatment:
Surgical Treatment:
Surgery is considered when conservative treatment fails after 6 to 12 weeks, or when there are signs of significant neurological compromise. Surgical options include:
At Fakeeh University Hospital Dubai, our spine surgery team offers the full range of minimally invasive and advanced surgical treatments for disc prolapse — with a focus on fast recovery and long-term outcomes.